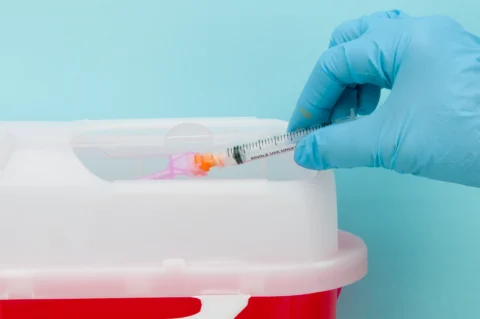
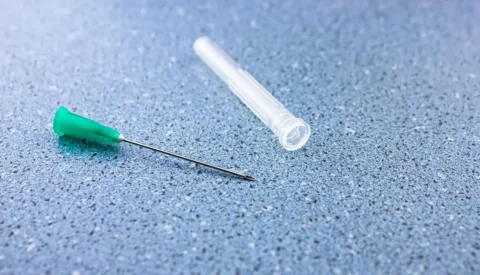
A Comprehensive Guide to the Evolution, Types, and Applications of Hypodermic Needles
Ever wonder how hypodermic needles came to be and the remarkable history behind their development?
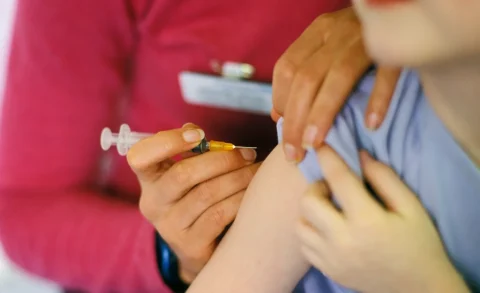
Devised in the mid-1800s, hypodermic needles revolutionized medicine by allowing for precise administration of drugs. No longer were medications restricted to oral or topical use – they could now be delivered directly into tissues and blood vessels.
Hypodermic needles have been essential in advancing fields like anesthesiology, pharmacology, and current medical procedures. Their miniature size and ability to penetrate the skin with minimal damage and pain have truly transformed health practices. There is no doubt that hypodermic needles rank among the most important medical tools ever created, and I’m thrilled to explore all aspects of these scientific wonders with you.
History and Evolution of Hypodermic Needles
In the early 1800s, some of the first primitive hypodermic needles were crafted from hollowed-out goose quills or glass tubes. An Irish doctor named Francis Rynd is credited with creating one of the first hypodermic syringes in 1844 using a goose quill and bladder. These early syringes were crude but represented an important first step.
As medicine advanced in the following decades, silver wires and chloride of lime were introduced to sterilize needles between uses. Glass hypodermic tubes eventually replaced quills and held medications more effectively. By the 1860s, metal needles began to replace glass, as they were stronger, less fragile, and could be produced on a larger scale.
Key breakthroughs were made in the late 1800s that led to the modern hypodermic needle.
In 1863, Charles Gabriel Pravaz created one of the first hypodermic syringes. It consisted of a glass tube attached to a metal needle at one end and a rubber bulb at the other end used to create suction and draw fluid into the syringe. Pravaz’s design revolutionized medicine by making hypodermic injections faster, easier, and less painful. In 1871, Alexander Wood invented the first metallic hollow needle.
Throughout this history, hypodermic needles grew thinner, stronger, safer, and easier to use. What started as a crude tool has become a precision medical device enabling treatment of a wide range of conditions. The evolution of hypodermic needles is a testament to human ingenuity and the progress of science.
Development of Syringes and Modern Hypodermic Needles
The invention of the hypodermic syringe was key to transforming hypodermic needles into the precision medical tools they are today. Previously, medications had to be loaded into needles by hand, which was tedious, imprecise, and unsafe. The development of the hypodermic syringe remedied these issues by allowing for easy, controlled loading and injection of drugs.
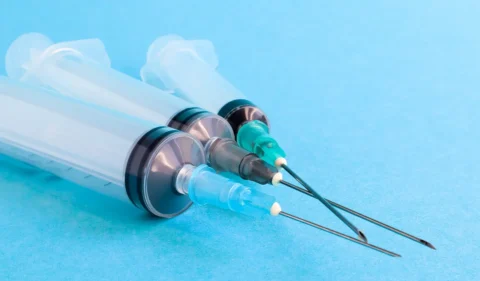
Modern hypodermic needles used in medical procedures continue to be micro-thin, precision-tapered stainless steel tubes attached to syringes. Specialized needles are also designed for different uses like drawing blood, infusing medications, or accessing vascular systems. New materials, coatings, and needle features help reduce friction, clogging, and tissue damage while expanding capabilities.
The evolution of the hypodermic syringe and continued progress with medical needles have been instrumental in enabling many disease treatments, medical procedures, and public health advancements that improve and save lives today. No history of hypodermic needles would be complete without recognizing the key role that their seamless integration with syringes has played.
Advancements in Materials and Design of Hypodermic Needles
Other improvements in materials include the use of hypodermic tubing, which allowed for easier mass production of needles. New alloys were developed with greater hardness, flexibility, and heat treatment techniques to improve strength and prevent dulling. Coatings like Teflon, Parylene, and titanium nitride help reduce friction, clogging, and tissue trauma.
These advancements in materials have enabled significant improvements in needle design.
Thinner walls, tapered points, and curves/bends allow for reduced penetration force, decreased trauma, and access to new injection sites. Specialized needles have been created for different uses, including drawing blood, infusing chemotherapy drugs, accessing ports or arterial systems, and more. Automatic or safety features help prevent needlestick injuries.
High-quality, durable hypodermic needles that minimize damage while maximizing safety, precision, and versatility have truly transformed medical procedures. Thanks to progressive materials research and innovative designs, what was once a crude tool is now a highly engineered medical device.
Types of Hypodermic Needles and Their Applications
Let’s dive deeper and explore the main types of hypodermic needles and their applications in medicine.
Standard Hypodermic Needles
The standard hypodermic needle is a common rounded-tip needle used for intramuscular injections and subcutaneous injections. Sizes range from 18 to 36 gauge, with lower gauges indicating thicker needles. Standard needles are versatile and used to deliver a wide range of medications or fluids.
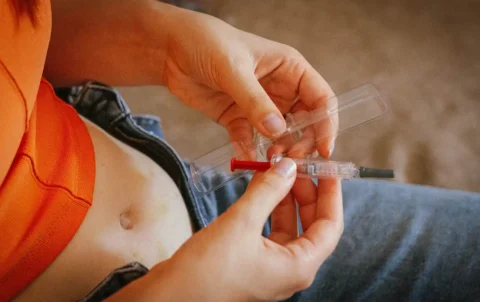
Insulin Needles
Insulin needles are fine, ultra-sharp needles designed specifically for injecting insulin. They are 29 gauge or finer to minimize discomfort from injections. The small size and precision tip allow for safer insulin delivery with less tissue damage.
Intravenous (IV) Needles
Intravenous (IV) therapy needles are used to access veins and administer IV fluids, medications, blood or blood products. They have a tapered tip to facilitate venous access while the thickness provides durability for multiple IV insertions. IV needles come in smaller gauges, often 20 to 24 gauge, for increased flexibility and reduced blood reflux.
Blunt Needles
In contrast, blunt needles have a rounded tip that does not penetrate the skin. They are used for blood drawing, establishing an intravenous line, or accessing ports. The dull tip eliminates the risk of accidental sticks from an exposed needle point. Blunt needles come in a range of gauges based on intended use.
Other less common types include spinal needles for lumbar punctures, epidural needles for administering epidural anesthesia, and catheter needles for placing intravenous catheters. The needle is selected based on factors such as gauge, length, tip configuration, material, and indication for use.
Hydra Needles
Hydra needles, or hydraulic needles, are hollow-bore needles with a hydraulic expandable tip. When fluid is injected into the needle, the tip expands to facilitate tissue dissection prior to collecting a cell or fluid sample. This allows for minimally invasive procedures with less damage to surrounding tissue.
Hydra needles were developed to improve techniques like amniocentesis, cyst aspiration, and draining abscesses. The expandable tip gains access to the targeted area while causing less trauma. It also seals around the internal diameter of the needle, creating suction to obtain a sample upon withdrawal of the needle. This helps yield a more representative sample with less contamination.
Benefits of hydra needles include:
| Minimized tissue damage | The expandable tip dilates tissue gradually rather than cutting, reducing damage to cells and structures. This leads to less bleeding, pain, and complications. |
| Improved sample quality | The sealed tip collects less contaminated, more intact samples with a higher cell yield and viability. This is useful for procedures like amniocentesis where sample quality is critical. |
| Safer procedures | Hydra needles help avoid complications from excess force, tearing tissue, or creating holes that do not seal properly. The controlled dilation and suction provide very targeted access and sample collection. |
| Reduced discomfort | By minimizing damage to tissue, hydra needles decrease pain, bleeding, and other acute side effects of procedures. Patients often report significantly less pain from hydra needle biopsies or fluid drainage. |
| Repeated use | Because they cause less trauma, hydra needles can sometimes be used multiple times in the same patient during a procedure. Some studies report re-using the same needle up to 3-5 times to collect additional samples. |
Adaptable Safety Needles and Preventing the Spread of Disease
In this section, we explore how disposable needles and adaptable safety needles have helped reduce the spread of disease.
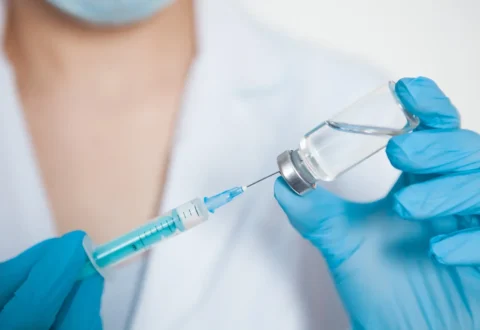
Disposable needles were introduced in the early 1900s and represented a major breakthrough in safety. Prior to disposables, needles were sterilized and reused, risking infection transmission between patients. Disposable needles ensured that each use involved a sterile, unused needle, vastly reducing disease spread. Made of materials like latex, glass, or stainless steel, disposable needles eliminated the dangers of reusing medical equipment on multiple patients.
Key benefits of disposable needles include:
Infection prevention. By providing a sterile needle for each use, disposables minimized the risk of transmitting bloodborne pathogens or other infections between patients. This helped reduce rates of HIV, hepatitis, and other diseases spread through medical care.
Improved sterility. It is difficult to effectively sterilize and disinfect needles between uses without some risk of re-contamination. Disposables dispose of needles after a single use, ensuring maximum sterility.
Cost-effectiveness. Although disposables added to waste, they reduced liability costs from infections as well as treatment costs for patients who became infected. This made them affordable and practical for widespread use.
Enhanced safety standards. The transition from reusing to disposable needles raised awareness of sterility protocols and safety practices in healthcare. It helped establish higher standards that continue improving patient safety today.
To further enhance safety, adaptable safety needles now include retractable blades, shields, or collapsible needle tips that Automatically cover the sharp point after use or when released. These needles help prevent injury from accidental sticks during handling, disposal, or setup.
| Key Types of Adaptable Safety Needles | Description |
| Retractable needles | The blade slides into the needle cannula after injection. |
| Sliding safety needles | A shield or collar slides over the needle tip when tension is released after injection. |
| Hinged safety needles | A hinged metal shield or collar folds over the needle tip when tension is relaxed. |
| Collapsible needle tips | The needle tip collapses in on itself after injection instead of leaving an exposed sharp edge. |
Safety needles, along with disposables, have been crucial in reducing hazardous exposures, disease spread, and accidental injuries throughout the medical field.
THE PERFECT NEEDLES FOR YOUR PATIENTS. CODE “20OFF” FOR 20% OFF YOUR FIRST ORDER!
FACE Med Store supplies countless doctors and clinics with all their supplies, including top-of-the-line hypodermic needles. Get your hypodermic needles at 20% off today!

Hypodermic Needles and Potential Allergic Reactions
Hypodermic needles, while important medical devices, do have the potential to trigger allergic reactions or sensitivities in some patients. This section explores the relationship between hypodermic needles and allergic responses.
Allergic reactions to needles can arise from several factors, including:
Materials: Certain needle materials like latex, nickel, or epoxy may cause allergic contact dermatitis or other material sensitivities in sensitive individuals. Stainless steel needles are often used as an alternative for those with metal allergies.
Drugs or fluids: The substances administered through needles, such as medications, contrast dyes, or blood/blood products, can trigger allergic or anaphylactic reactions in susceptible patients. These drugs or fluids come into direct contact with tissues through needle injection.
Sterilants: Chemical sterilants used to disinfect needles may be irritating or allergenic for those with sensitivities. Not all sterilants cause issues, so alternatives can often be used when needed.
Repeated use: While rare, some people can develop allergic contact dermatitis or other hypersensitivity reactions to needles due to repeated skin punctures over time, especially in areas frequently accessed like hands or arms. Using alternate sites or needle-free options may help in these cases.
Psychogenic: Occasionally, an anxiety-related psychosomatic reaction misperceived as an allergy can occur with needle use. Reassuring patients, using distraction techniques, or numbing the area can help in these situations.
Symptoms of an allergic reaction to needles include redness, swelling, itching, hives, and skin irritation at the injection site. More severe anaphylaxis is rare but can include dizziness, swelling beyond the site, fast heart rate, and low blood pressure. In high-risk patients, epinephrine, antihistamines, corticosteroids and IV fluids may be required to treat anaphylaxis.
To prevent allergic reactions, assessing patients for material sensitivities prior to procedures is important. Using alternative needle materials or needle-free options when possible can minimize risks. Proper sterilization techniques, clinical judgment, and close monitoring also help reduce the likelihood of hypersensitivity events.
While not very common, some individuals do develop allergic sensitivities or even anaphylaxis in response to hypodermic needles, needle materials, irrigating fluids or medications administered through them. Awareness of potential allergic risks, alternative options when available and close management help ensure safe medical care for these patients.
Conclusion
Hypodermic needles have undoubtedly revolutionized medicine since their introduction in the mid-1800s. Developed from crude tools into high-tech instruments, hypodermic needles and the hypodermic syringes they partner with have enabled tremendous progress in treatment, prevention, and public health. By making once invasive and painful procedures faster, safer, and less traumatic, hypodermic needles have helped enhance standards of care, extend lifespans, and improve quality of life for people around the globe.
Packed with innovation, these revolutionary hydra needles pierce boundaries while soothing pain—enabling procedures once thought impossible.