Regenerative medicine therapies are often regarded as alternative methods to surgical procedures when it comes to managing disorders like osteoarthritis. They’re often compared to each other when it comes to their efficacy and safety profiles. Some of the most popular treatments for osteoarthritis include shoulder arthroplasty, autologous stem cells, PRP and viscosupplementation.
So among shoulder arthroplasty, autologous stem cells, PRP, and viscosupplementation, what’s the best for osteoarthritis? There’s no exact answer to these since among these options, the best treatment is what will work in the management of the different symptoms of osteoarthritis and what works for each person. These procedures may even be used in combination with each other so choosing what will work best for you is still a matter of patient’s preference as well as provider’s judgment.
Treating Osteoarthritis: How Can It Be Done and What Are Your Options?
Osteoarthritis of the shoulder is a condition characterized by joint pain and stiffness. This is due to the degeneration of the thin covering at the ends of the bones that serve as a cushion for the friction between the bones known as the articular cartilage.
As with other diseases, the first step in managing osteoarthritis is to get the proper diagnosis to make sure the available treatment options will work. The available treatment options include:
- Shoulder Arthroplasty – Shoulder arthroplasty is an arthroscopic surgery where damaged tissue is removed and shoulder replacement is done via a prosthesis.
- Autologous Stem Cells – Autologous stem cells entail the use of mesenchymal stem cells from sources such as bone marrow, adipose tissue, and umbilical cord. They have immunosuppressive and anti-inflammatory properties.
- Platelet-Rich Plasma Injections – Platelet-rich plasma injections are an autologous blood product that takes advantage of the regenerating effects of growth factors and pro-inflammatory cytokines to promote improvements in pain and other symptoms of shoulder arthroplasty.
- Viscosupplementation – Viscosupplementation injections are one of the biologic injections of regenerative medicine that entail the administration of hyaluronic acid for arthritis treatment.
Shoulder Arthroplasty
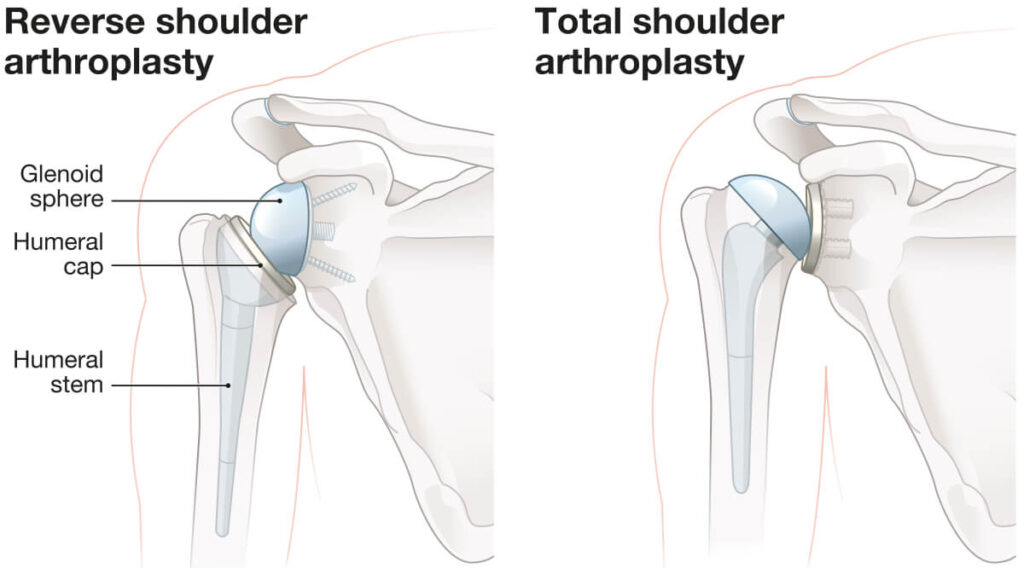
Shoulder arthroplasty is one of the invasive procedures that can be done against osteoarthritis of the shoulder. Done by orthopedic surgeons, shoulder arthroplasty involves the replacement of the shoulder with artificial equipment called a prosthesis.
1) How It’s Done
An incision around 16 inches in length will be done in the anterior portion of the shoulders to open up the shoulder. Pins will then be drilled as a guide to cut off the head of the humerus (which is the bone of the arm) using a surgical saw. The pins will then be removed together with the head that was cut.
The damaged cartilage in the exposed glenoid fossa or the bone socket will then be scraped off. The socket will then be drilled with a hole to which implants will be placed along with another implant in the arm. It’s up to the surgeon if these implants will be cemented in place.
2) Efficacy
Except for patients with severe injury or arthritis who would benefit more from reverse shoulder replacement, shoulder arthroplasty is ideal for patients with less damaged rotator cuff muscles. This procedure has a high success rate, and those who undergo this operation are typically able to go back to their active lifestyles.
Shoulder replacement prostheses are estimated to last 15 to 20 years (or even longer, depending on an individual). It has a failure rate of 1% per year which is brought by the “wearing out” of the prosthesis, characterized by cracking or loosening.
3) Safety
The survival rate for this surgical procedure is high, with a 10-year survival rate of up to 90 percent. In fact, a study where patients who underwent anatomic total shoulder arthroplasty were followed up after 5 years showed that 10.3% complications occur per procedure or a total of 345 complications in 3,360 shoulders.
Common complications associated with this surgical procedure include:
- Component loosening
- Glenoid wear
- Instability
- Rotator cuff tear
- Periprosthetic fracture
- Neural injury
- Infection
- Hematoma
- Deltoid injury
- Deep venous thrombosis
4) The Need For Rehabilitation
After the surgery, the patient will be placed on a sling for 4 to 6 weeks after surgery to facilitate healing of the shoulders. Additionally, the use of regional anesthesia may numb the area for 12 to 18 hours after the procedure.
Physical therapy is needed to further facilitate the patient’s recovery. Physical therapists will constantly visit the patient during his or her stay in the hospital to reinforce the exercises prescribed by the doctor for regaining full shoulder functionality.
Autologous Stem Cells: What You Need to Know
Stem cell therapy is one of the injection therapies that may be done in an arthritic joint. A single injection of this therapy contains stem cells collected from bone marrow, adipose tissue, or umbilical cord. It works through regenerative and anti-inflammatory means and has been proven to be as safe and as effective as other treatments.
1) How It’s Done
The patient is sedated and brought to the surgery room where injection sites are visualized using imaging techniques such as x-ray. Blood will then be taken from the patient, which will undergo rounds of centrifugation to concentrate the stem cells.
Upon concentration of stem cells, the processed formulation will then be injected into the visualized injection sites. When the injection is done, the injection sites will then be closed using stitches.
The board-certified orthopedic surgeon will then review the procedure again and the patient will be brought to the recovery room where they’ll stay for a few hours then immediately go home afterward.
2) How It Works
Stem cells can differentiate (i.e. mature and develop) into cell lines necessary for the healing of the shoulders. These cells include osteogenic and chondrogenic cell lines, which are cells for the bone and cartilage, leading to the regeneration of these components of the shoulders.
However, more than this regenerative capacity, it’s speculated that the anti-inflammatory effect of autologous adult stem cells is the more prevailing factor as to the healing capacity of injections containing this biologic factor.
3) Efficacy
Not enough studies have been done to prove the efficacy of stem cell therapy for shoulder osteoarthritis to draw conclusions as to its efficacy. This is because shoulder osteoarthritis is often underdiagnosed. However, the results of studies that have already been published are promising, proving the therapeutic potential of stem cells in relieving symptoms of shoulder osteoarthritis.
4) Safety
Animal studies and clinical trials have demonstrated the safety of the use of stem cells for shoulder osteoarthritis, as they’ve shown that this procedure resulted in no major side effects, especially because they’re made from natural products and derived from a person’s own blood.
Moreover, the oncogenic risk associated with the use of mesenchymal stem cells isn’t due to the formulation itself but due to the contamination of the cell lines by malignant cells.
Platelet-Rich Plasma
Platelet-rich plasma injection is one of the alternative, non-surgical options that have arisen in the advent of regenerative medicine. Its efficacy is highly dependent on the concentration of platelets that secrete the growth factors necessary for this procedure.
1) How It’s Done
The formulation for platelet-rich plasma injections is derived from the patient’s own blood. Several rounds of centrifugation will be done to separate the blood components and increase the concentration of platelets comparably to the natural status of blood.
Upon collection of the formulation, the healthcare professional will then visualize the damaged tissue via imaging techniques such as ultrasonography, which is best done with the modified Crass position. They’ll then sanitize and numb the area to which the platelet-rich plasma injections will be administered, still guided by ultrasonography or other imaging techniques.
2) How It Works
A platelet-rich plasma injection works by mediating the natural wound healing process of the body. It has anti-inflammatory and chondroprotective properties, as well as potential regenerative effects brought by the concentration of growth factor secreted by the platelets present in the formulation.
Some of the growth factors present in the platelet-rich plasma include platelet-derived growth factor, vascular endothelial growth factor, among others. These growth factors have cell proliferative, angiogenic (production of new blood vessels), and cell differentiation properties.
3) Efficacy
A study comparing platelet-rich plasma injections with steroid injections has shown the effectiveness of PRP injections in providing significant improvements in the quality of life of patients. It has even proven to be superior over steroid injections attributed to its regenerative capacity bringing longer-lasting results.
4) Safety
Platelet-rich plasma injections have a good safety profile, owing to the fact that they’re natural products derived from the patient’s own blood. Because of this, the risk of manifesting allergic reactions and contracting communicable diseases is minimized.
Some of the known side effects of platelet-rich plasma injections are mild and aren’t attributed to the formulation itself but usually to the way the healthcare professional handles the procedure. These side effects are injection site-related,including pain, redness, swelling, nerve damage, and tissue damage, which all typically resolve on their own.
Viscosupplementation
Visco injections are a kind of biologic injection treatment that entails the administration of hyaluronic acid-containing injections administered once a week for 3 weeks. It’s proven safe and effective as evidenced by its FDA approval for general use in 1997.
1) How It’s Done
As with the other two biologic treatments, viscosupplementation may also involve ultrasound-guided injections or performed in a blinded injection where no imaging technique is used but palpation and clinical experience. The area will then be sanitized and injections will be administered in a manner where suctions are created.
2) How It Works
Hyaluronic acid is a necessary building block of proteoglycans, the substance that helps trap water and provides compressive strength to the articular cartilage. Responsible for giving lubrication and cushion, hyaluronic acid helps the joints work more smoothly.
Viscosupplementation injections provide an additional source of hyaluronic acid to the joints, especially when they’re thinned out as a result of osteoarthritis. Hyaluronic acid supplemented by visco injections also have anti-inflammatory and anti-oxidative stress properties that help relieve the symptoms of osteoarthritis.
3) Efficacy
Intra-articular injection of hyaluronic acid (IA-HA injection) was proven by studies and clinical trials to be helpful in improving symptoms of osteoarthritis, such as pain and function. In fact, these studies and clinical trials have also pointed towards the superiority of IA-HA injection combined with arthrocentesis.
4) Safety
Studies and clinical trials have also shown a good safety profile for viscosupplementation, which led to its FDA approval in 1997. The local adverse reactions rate is noted to be between only 2% to 4%.
Side effects of this procedure are minimal and subside on their own. These side effects include minor pain at the injection site, minor buildup of joint fluid, and, less frequently, increased inflammation.
A Good Option: Educational Video Courses
A patient’s decision on choosing among the wide variety of treatment options on certain diseases must be guided by a physician through proper patient education. In turn, proper patient education is facilitated by a healthcare professional with a good understanding of how a treatment modality works.
Taking video courses are good ways to expand a healthcare professional’s knowledge on treatment modalities and may help in their professional growth.
Examples of these video courses like the ones offered by FACE Med Store are “Platelet Rich Plasma (PRP) Platelet Rich Fibrin Matrix (PRFM) in Regenerative Medicine Video Course” and “PRP for Sexual Health Including Live Vaginal and Penile Injection Training” as well as educational videos on osteoarthritis treatments would be useful for both patient and provider.
In these video courses, PRP, PRFM and how they bring benefits to osteoarthritis patients are thoroughly discussed by professionals like Lanna Cheuck, DO, FACS, a board-certified urologic surgeon.
Shop at FACE Med Store for the Best Medical Products
-
 10 Kit PRP Centrifuge Starter Bundle
10 Kit PRP Centrifuge Starter Bundle -
 20 Kit PRP Centrifuge Starter Bundle
20 Kit PRP Centrifuge Starter Bundle -
 Butterfly Needle – 23G 3/4 in. x 12 in. with sliding safety shield- Box of 100
Butterfly Needle – 23G 3/4 in. x 12 in. with sliding safety shield- Box of 100 -
 Butterfly Needle – 25G 3/4 in. x 12 in. with sliding safety shield- Box of 100
Butterfly Needle – 25G 3/4 in. x 12 in. with sliding safety shield- Box of 100 -
 CM-7S PRP Plus
CM-7S PRP Plus -
 30 Gauge 13mm (0.5 inch) Hypodermic needles
30 Gauge 13mm (0.5 inch) Hypodermic needles -
 32 Gauge 13mm (0.5 inch) Hypodermic needles
32 Gauge 13mm (0.5 inch) Hypodermic needles -
 34 Gauge 4mm (0.16 inch) Hypodermic needles
34 Gauge 4mm (0.16 inch) Hypodermic needles -
 32 Gauge 4mm (0.16 inch) Hypodermic needles
32 Gauge 4mm (0.16 inch) Hypodermic needles
Comparing the efficacy and safety of the available treatments allows patients to make informed decisions about the treatment they want to undergo. Patient preference guided by advice from a healthcare professional helps determine what the best treatment for osteoarthritis is.
At FACE Med Store, we offer the best medical products for hair regrowth and skin rejuvenation. Our friendly customer service team can also provide specific product information and explanations to let our clients know which medical products work best for their condition. Contact us today at info@facemedstore.com to get to know our products better.
Learn More: How Many Times Can You Have A PRP Injection To Repair A Meniscus?