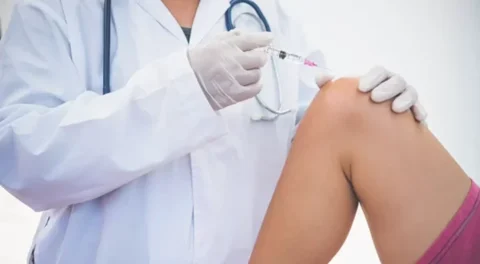
Platelets, the fundamental element of primary hemostasis, are also known to be reservoirs for many growth factors (GFs), which they store in their α-granules. Platelet aggregation and activation, after vascular damage, results in the release of several GFs that may affect the chemotaxis, proliferation, and differentiation of mesenchymal stem cells (MSCs) or other committed cells during the process of tissue repair and healing.
The GFs released from platelets include platelet-derived growth factors (PDGFs), changing growth factor-beta (TGF-β), vascular endothelial growth factor (VEGF), epidermal growth factor (EGF), fibroblast growth factor (FGF) and insulin-like growth factors (IGFs).
What Do The Studies Say About PRP?
To explore the possibility that platelet-rich plasma (PRP) could provide an autologous source of these essential GFs that benefit bone and soft tissue healing, many clinical and experimental studies dealing with the effects of PRP have been conducted. However, the benefit of PRP on bone formation is a controversial subject. While a report suggested a stimulatory impact with the addition of PRP, others have observed no improvement or have detected even inhibitory effects.
Although the lack of standardization in application across these studies, including differences in the preparation method or dosage of PRP, biomaterials, species, implantation sites, and cell types, may have contributed to the inconsistent results, its hypothesized that the differences in GF composition among PRPs could lead to this discrepancy.
How Does PRP Effect Growth Factors?
Findings indicated that PRP induced proliferation in a dose-dependent manner. The addition of 10% PRP to the culture medium produced marked cell proliferation in vitro; this result was congruent with the findings of previous studies. Because higher concentration (30%) of PRP did not promote proliferation, as compared to controls, 10% PRP may be optimal for the experimental ex vivo expansion of mesenchymal stem cells (HMSCs).
Few studies have suggested the presence of negative regulators in PRP, such as thrombospondin, but the reason for the antiproliferative effect of high-concentration-PRP is not apparent.
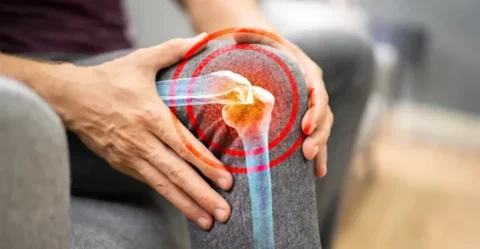
In a study, PRP suppressed the alkaline phosphatase (ALP) activity of mesenchymal stem cells (MSCs). Some studies have reported similar results in that PRP increased migration and proliferation, but reduced the osteogenic differentiation of bone marrow-derived MSCs in vitro.
However, in this study, activated platelet-poor plasma (aPPP) did not suppress ALP activity at any concentration; therefore, these inhibitory effects may be associated with substances that are derived from platelets.
What Are The Results Of Pep Factor?
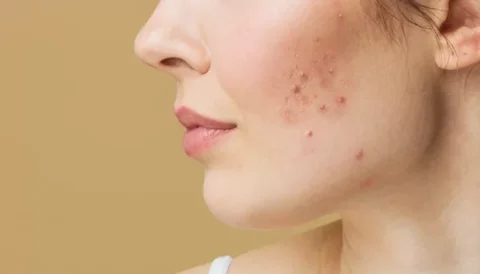
Pep Factor has consistent results among clients and has provided many people with youthful skin as well as renewed growth of hair. Researchers have made several innovations in molecular medicine and valuable ingredients for their delivery systems. Researchers are also researching more useful, cost-effective, and easy methods for skin and scalp cosmetics.
Our Pep Factor is created from the start with the purpose of magnifying Fibroblast. We want our kit to provide the maximum amount of benefits for what our clients need. FGF is responsible for the regeneration of tissue, including skin and hair follicles. UMA’s research laboratory has designed this unique formula. FGF also directs a range of multiple biological functions, including cellular proliferation, durability migration.