For information only. Not meant as advice in any form. Please consult your medical professional.
Dermal fillers are generally a safe and low-risk cosmetic procedure for facial rejuvenation and anti-wrinkle treatment. However, while the risk for adverse effects is minimal, there are still some cases where an injectable filler may cause late inflammatory reactions and knowing how to manage it is important so you can help your patients.
So how effective are colchicine and Indocin for late-onset nodules with dermal filler injections? Colchicine and Indocin are common drug recommendations for inflammation, swelling, tenderness, and pain. There’s a study that suggests that patients with post-filler nodules may benefit from colchicine. Meanwhile, there is limited evidence on whether Indocin can be taken but with its anti-inflammatory effects, it may also be recommended while practicing caution.
Treating Post-Filler Delayed Onset Nodules With Colchicine and Indocin Drugs
Side effects from dermal filler treatments are not completely uncommon. Every patient reacts differently to the cosmetic injectable depending on their medical history, current health, type of filler product, injection depth, and how much volume was added. Normally, most reactions, such as swelling, bruising, and redness, can last for a few days and subside on their own.
However, there’s also a small possibility that the injectable will trigger a delayed inflammatory reaction. This may lead to the development of a foreign body granuloma or nodules that may appear within weeks or months after the injection. This type of complication is not particularly life-threatening but it may cause discomfort for the patient.
Most nodules from hyaluronic acid fillers may resolve on their own since the injected material is temporary and gradually dissolves in the body. However, reactions from a semi-permanent filler will not easily go away on their own. In these rare cases, the administration of systemic steroids or antibiotics, such as colchicine and indocin medications, may be done to help manage the nodules.
All About Colchicine and Indocin Medications and Their Common Applications
Treating a delayed foreign body reaction from dermal fillers typically requires intralesional steroid injections. This involves direct administration of a corticosteroid medicine into the affected site to stop the inflammatory activities of the cells, fibroblasts, and macrophages that cause the appearance of skin lesions, nodules, and granulomas.
For persistent nodules, oral medications such as colchicine and indocin may be recommended to aid in the recovery of the patient. They’re usually prescribed in small doses and may be taken for a few weeks until the nodules are gone.
What Is Oral Colchicine?
Colchicine is an alkaloid that’s naturally derived from the plant called Colchicum autumnale. It’s usually prescribed to treat inflammatory medical disorders such as gout, Familial Mediterranean Fever, and recurrent pericarditis. When taken orally, this drug has been shown to inhibit uric acid production which often leads to pain and inflammation in the joints.
Over the years, colchicine has also been closely studied for the treatment of various skin conditions. In a study, this medication showed promise in managing inflammatory skin disorders such as psoriasis, acne vulgaris, perforating dermatoses, and pustular dermatoses. The research suggests that colchicine may be used as a second- or third-line treatment for such conditions.
What Is Oral Indocin?
Indocin is a common brand name for the non-steroidal anti-inflammatory drug known as indomethacin. Similar to colchicine, this medication is widely used to manage symptoms of gout, osteoarthritis, rheumatoid arthritis, and other inflammatory conditions.
It’s usually taken orally and it works by blocking the release of certain substances that cause inflammation. Unlike colchicine drugs, there is limited evidence to support the successful use of Indocin for skin problems.
How Effective Are These Anti-Inflammatory Medications For Post-Filler Nodule Care?
Both colchicine and Indocin medications may be considered systemic therapy for delayed onset nodules or granulomas from soft tissue filler injections. However, the availability of clinical findings that support the successful use of these drugs for filler-induced nodules is still limited.
Only colchicine has already been tried and tested for the management of foreign body granulomas from injectables. In a 2007 study, a group of researchers treated a female patient who developed nodules on her face after her filler injections. The medicine was administered alongside intralesional steroid injections to provide better results.
The recommended dosage of colchicine may vary depending on the severity of the nodule present. In a separate study, an author suggested that using 0.6 mg of oral colchicine every 12 hours for at least a week may provide good results for controlling the inflammation at the affected site.
On the other hand, there are no available studies yet to prove the effectiveness of indocin as a treatment for late onset nodules from injectable fillers. While they’re usually prescribed for various inflammatory conditions, using them for granulomas from dermal fillers should be done with caution. They may be recommended as an adjunct therapy but not a primary treatment for delayed onset nodules.
Possible Side Effects of Colchicine and Indocin Tablets
Before prescribing medication for dermal filler patients, it’s important to understand and discuss the side effects that they may have. Taking oral colchicine and indocin tablets may cause reactions such as:
- Nausea
- Vomiting
- Diarrhea
- Upset stomach
- Abdomen pain
- Drowsiness
- Dizziness
- Constipation
- High blood pressure
It’s important to recommend the medications for treating nodules in moderation to avoid serious complications. Make sure to closely monitor your patients and provide immediate medical help if an adverse reaction, such as ulcers, stomach bleeding, muscle weakness, or unexplained stiff neck, happens.
Who is Not Suited To Take Colchicine and Indocin?
Just as an initial consultation is important before injecting dermal fillers, it’s also crucial that you examine a patient before prescribing any medication for their nodules. Colchicine and Indocin may interact with other medications so you should check if they’re currently taking other drugs. As a precaution, patients who are taking these medications may not be suited for colchicine and Indocin:
- Antifungal drugs such as ketoconazole and itraconazole
- ACE inhibitors like benazepril, captopril, and enalapril
- Beta-blocker medications such as atenolol, labetalol, and metoprolol
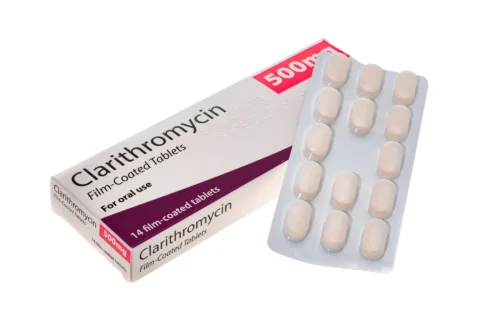
- Antibiotics like telithromycin or clarithromycin
- Antidepressant drugs
- Cholesterol medications
- Heart medicines such as verapamil and diltiazem
Additionally, you should assess their current health prior to prescribing the anti-inflammatory medications. Colchicine and Indocin are typically not prescribed to individuals with the following medical conditions:
- Patients with a history of asthma, heart failure, seizure, or kidney or liver disease
- Patients with a blood disorder, such as having low platelet counts or low white and red blood cells
- Patients with known allergies to colchicine or indomethacin
- Patients who are pregnant, breastfeeding, or trying to have a baby
Other Medications That May Help With Late Onset Nodules From Fillers
Systemic therapy and the use of other oral medications are usually the first-line treatment for late onset nodules and granulomas from cosmetic fillers. If a patient should receive drugs for management of the delayed side effects, the dosage should be carefully planned. You should also set expectations as taking medicine may take some time before it fully clears the nodules.
Aside from colchicine and indomethacin medications, here are other treatment options that may help:
1. Antihistamine medications
If persistent nodules are accompanied by hypersensitivity or allergic reaction, an antihistamine medication may also be recommended to the patient. These drugs are specifically used to treat symptoms, such as swelling and itching, and may help with delayed inflammatory reactions from dermal fillers. Some common antihistamines that may be prescribed are cetirizine and loratadine.
2. Allopurinol
This drug belongs to the same class as colchicine and it’s used to also treat gout, arthritis, and kidney stones. However, a study shows that allopurinol can provide promising effects for the management of foreign body reactions from injectable filler treatments. It’s usually prescribed at a high dose of 300 to 600 mg/d and may be taken at least twice a day.
3. 5-fluorouracil
This medication is an antibiotic agent which helps stop bacterial infections and inhibits the action of microorganisms and other substances that lead to delayed nodules. It’s usually given in a series of intralesional injections for at least 2 to 4 weeks until the granulomas and nodules are resolved. They may be administered on their own or along with other intralesional corticosteroids.
4. Hydroxychloroquine
While this medication is commonly used to treat malaria, it also contains several anti-inflammatory and anti-viral properties that may be helpful for managing late onset filler nodules. They may be suggested as part of a treatment plan to reverse the inflammatory reactions from the fillers.
5. Isotretinoin
Sometimes, late onset nodules may also cause erythema or redness of the skin due to persistent inflammation. If this happens, oral isotretinoin may be recommended as a treatment. This medication is generally used to treat moderate to severe nodular or cystic acne and it may help manage the redness and inflammation of the affected area.
6. Topical ointments
Medicated creams such as tacrolimus and pimecrolimus may also be helpful for treating delayed onset nodules caused by hypersensitivity reactions from fillers. These topical ointments have potent anti-inflammatory actions and may help improve the appearance of nodules on the skin.
Types of Nodules from Dermal Fillers
The choice of treatment of delayed nodules from dermal fillers may vary depending on the diagnosis. Generally, there are three types of nodular inflammatory reactions according to their causes:
- Foreign body reactions: These granulomatous nodules happen as a result of inflammation in the treatment area. This is usually a response to the trauma from the injection, the amount of filler material placed, the composition of the injectable, and how deep the substance was injected.
- Immune-mediated or hypersensitivity reactions: Delayed onset nodules may also be caused by allergic reactions to the filler material. Usually, this type of inflammatory reaction happens within a few months after the injections. Its common symptoms are the appearance of nodules, edema, redness, and itching.
- Infections: Some nodules may also be triggered by a bacterial, viral, or fungal infection. This can happen when the filler material has been contaminated prior to injections. They may manifest on the skin as nodules, abscesses, or granulomatous reactions.
Other Ways to Treat Nodules From Dermal Fillers
Most oral antibiotics are an effective initial treatment for early diagnosed nodules. However, if the inflammatory reactions have progressed or if they’re not responsive to medications, there are other better-suited treatments that may help:
1. Excision with Hyaluronidase Injections
Hyaluronidase is an effective dermal filler removal treatment. It consists of an enzyme that can help facilitate the breakdown of the injected material so it’ll be quickly absorbed by the body. They’re typically done for nodules caused by misplaced fillers and bacterial infections.
According to a study, a patient will typically need around 30 to 300 units of intralesional hyaluronidase injections per nodule. They may receive at least 2 to 3 rounds of injections until the nodules are fully dissolved.
2. Surgical Treatment
If nodules are still present after systemic therapy, a patient may be required to get surgical excision. Since this treatment is invasive, a thorough diagnosis with scans of the nodules should be performed before doing the procedure. Typically, surgery is only recommended when a granuloma or abscess is present. It should only be recommended as a last resort since it has risks of post-surgical scars.
Ways to Prevent the Risk of Delayed Nodule Reactions
It’s the injector’s responsibility to ensure that their patients receive comfortable and safe dermal filler procedures. Here are some helpful measures that can help minimize the risks of a delayed inflammatory reaction while ensuring a successful treatment:
- Have enough knowledge of facial anatomy and know how to determine the areas where fillers can be injected that can reduce the risks of nodules.
- Wash your hands and wear clean surgical gloves before starting the procedure.
- Make sure to use clean and sterile injection tools and instruments to avoid filler contamination.
- Place small amounts of fillers slowly in the desired treatment area. This will help avoid overfilling the site with volume to minimize post-procedure lumps and nodules.
- Massage the treated area to help evenly distribute the filler and avoid any lumps after the injection.
Shop High-Quality Medical Tools for Dermal Filler Treatments at FACE Med Store
Taking colchicine and Indocin medications are one of the methods that may help manage late onset nodules from dermal fillers. However, prevention is always better than cure and as a plastic surgeon or cosmetic provider, you should take proactive steps to minimize the risks of delayed inflammatory reactions from injectables.
At FACE Med Store, we offer a wide selection of high-quality, medical-grade tools and supplies that can be used to execute safe and effective dermal filler injections. We’re proud to be a trusted partner of many aesthetic clinics and medical practices around the country. To know more about our services, or to inquire about our stocks, call us today.